When we think of fertility, reproductive hormones like estrogen and progesterone may come to mind. But these hormones rely heavily on metabolic health to function properly. Therefore, how your body manages blood sugar and insulin can influence ovulation, egg quality, implantation, and even success rates for fertility treatments like IVF.
Understanding how blood sugar and insulin interact, and how daily habits influence them, offers a powerful yet often overlooked way to support reproductive health.
Blood Sugar and Insulin: A Foundational Relationship
Glucose is the body’s main source of energy. After eating, glucose enters the bloodstream and raises blood sugar, which stimulates the release of the insulin from the pancreas. Insulin is a hormone that acts like a transporter, allowing glucose to move into cells where it can be used for energy or stored for later use.
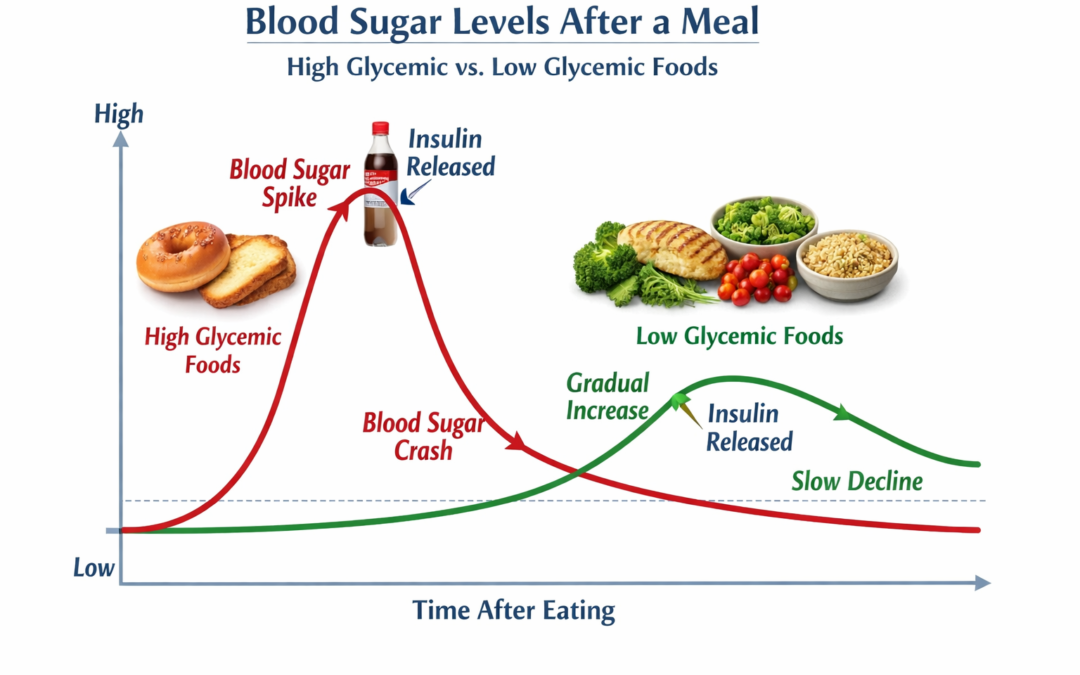
In a balanced system, blood sugar rises after meals and insulin is released to move that glucose into cells to bring blood sugar levels back into range. Ideally, a visual representation of this would look like a bell shape; a gentle slope upwards, rounded at the top and a gentle slope back down.
Issues can arise when this visual representation looks more like a steep mountain; a sharp incline upwards and a sharp drop downwards. Repeated blood sugar spikes and rapid drops keep insulin levels elevated, which gradually reduces cellular responsiveness to insulin, increasing the risk of insulin resistance.This can occur long before blood sugar levels appear abnormal on blood work.
Insulin Resistance and Fertility
Insulin resistance develops when cells respond less effectively to insulin, prompting the pancreas to produce higher levels to maintain normal blood sugar. This compensation can mask blood sugar dysregulation for years, making insulin resistance easy to miss.
Chronically elevated insulin has important implications for reproductive health. Insulin interacts closely with reproductive hormones and can disrupt signaling between the brain, ovaries, and uterus.
Elevated insulin levels can contribute to:
- Irregular ovulation and menstrual cycles due to hormonal imbalances
- Impaired egg maturation and egg quality
- Chronic inflammation – impacting the uterine environment & implantation
- Increased risk of pregnancy losses or complications
Research has shown that individuals with insulin resistance undergoing IVF may experience lower implantation and pregnancy rates compared to insulin-sensitive individuals, even when embryo quality is comparable. This suggests that metabolic health plays a critical role not only in egg development, but also in creating a supportive environment for implantation and early pregnancy.
Insulin resistance is a well-known driver of Polycystic Ovarian Syndrome (PCOS), which is characterized by symptoms of hormonal imbalance and ovulatory dysfunction. However, even in individuals without PCOS, elevated insulin can contribute to subtle hormonal disruptions, low-grade inflammation, and impaired metabolic signaling that negatively impact reproductive function.
How Food & Daily Habits Influence Blood Sugar
Not only does what and how we eat impact blood sugar and insulin levels, but also how we move and treat our bodies:
- Refined carbohydrates and added sugars (such as white bread, crackers, baked goods, sugary drinks, etc.) are digested quickly and tend to cause rapid spikes in blood sugar. These spikes are often followed by sharp drops, which can trigger fatigue, cravings, and a cycle of frequent snacking. These foods are generally high on the Glycemic Index.
- Protein slows digestion and reduces the speed at which glucose enters the bloodstream. Including adequate protein at meals helps blunt blood sugar spikes, supports satiety, and reduces post-meal crashes.
- Healthy fat further slows digestion and carbohydrate absorption, contributing to a more gradual rise in blood sugar and a steadier insulin response.
- Fiber-rich carbohydrates (such as vegetables, legumes, whole grains, nuts, and seeds) slow glucose absorption and improves insulin sensitivity, supporting more stable blood sugar over time. These foods are lower to moderate on the Glycemic Index.
- Meal size and composition matter. A “balanced” meal includes a good ratio of protein, fat and fiber-rich carbs. Meals that are too small or imbalanced may lead to blood sugar dips and increased hunger shortly after eating. While larger, balanced meals help maintain steady energy and glucose levels.
- Eating patterns also play a role. Skipping meals, grazing throughout the day, or relying heavily on snacks can keep blood sugar and insulin levels elevated which contributes to instability and insulin resistance.
- Gentle movement like walking after a meal will fire up your muscles and support digestion to use up that glucose
- Daily stressors will elevate cortisol and adrenalin – stress hormones that raise blood sugar and in turn, insulin. Being aware of and supporting your stress levels and nervous system are other ways you can keep blood sugar and insulin regulated.
Together, these factors highlight that blood sugar regulation is less about eliminating carbohydrates and more about creating balanced, nourishing meals and habits that support metabolic, reproductive and nervous system health.
A Supportive Path Forward
Although it’s clear that blood sugar and insulin regulation are foundational aspects of fertility, they are still often overlooked. Making changes in these areas can feel overwhelming during an already stressful fertility journey. But even small, consistent changes can have a meaningful effect on hormone signaling, ovulation, overall fertility and pregnancy outcomes.
For many individuals, attempting to navigate nutrition, lifestyle changes, and fertility care simultaneously can feel overwhelming. This is where working with a practitioner knowledgeable in nutrition with a holistic lens can help translate this information into a personalized, sustainable approach that supports your unique metabolic, reproductive and total body health.
Shannon McKirdy
Registered Holistic Nutrition Practitioner (RHNP)
References
Xu, J., et al. (2012). Insulin resistance is associated with decreased implantation and pregnancy rates in women undergoing in vitro fertilization. Fertility and Sterility, 98(4), 1037–1042.
Coviello, M., Muscogiuri, G., et al. (2018). Inositol and insulin resistance in reproductive health. Endocrine, 59(2), 269–279.
American Society for Reproductive Medicine. (2023). Metabolic factors and fertility outcomes.
Dunaif, A. (2006). Insulin resistance and the polycystic ovary syndrome: Mechanism and implications for pathogenesis. Endocrine Reviews, 27(7), 774–800.
Chavarro, J. E., Rich-Edwards, J. W., Rosner, B. A., & Willett, W. C. (2007). Diet and lifestyle in the prevention of ovulatory disorder infertility. Obstetrics & Gynecology, 110(5), 1050–1058.
Broughton, D. E., & Moley, K. H. (2017). Obesity and female infertility: Potential mediators of obesity’s impact. Fertility and Sterility, 107(4), 840–847.